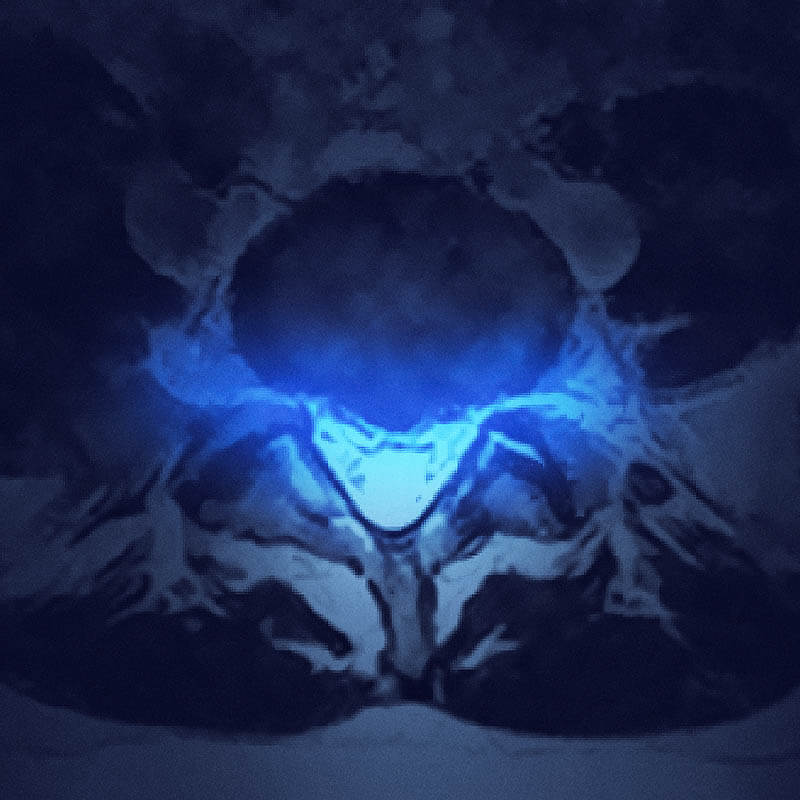
Comprehensive Diagnosis & Treatment of Herniated Discs
Also known as a slipped disc, a herniated disc is a common condition that typically affects patients between ages 20 and 50. Most cases resolve without treatment. Some herniated discs can result in extreme pain, numbness, weakness, muscle spasms, difficulty walking, and even a rare and serious condition known as Cauda Equine Syndrome, which affects bladder function.
Treatment Options
In most cases, surgery is not necessary to treat a herniated disc. Patients often find relief with functional and regenerative medical treatments, pain management or physical therapy to improve the strength and flexibility in the back, torso, and limbs.
In the rare case that surgery is required, the standard operation is microdiscectomy, a minimally invasive surgery that can be done on an outpatient basis.